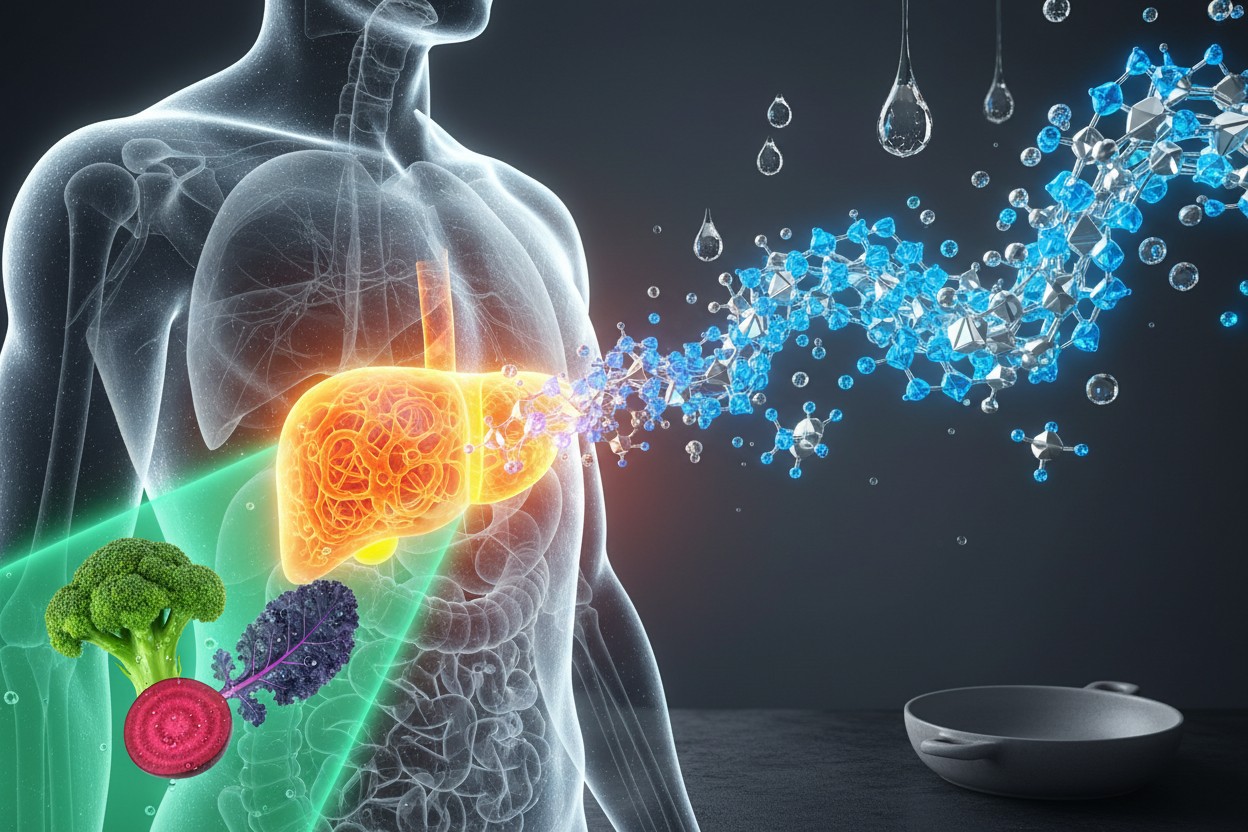
Diet as defense: How everyday foods could disarm deadly bacteria
04/10/2026 / By Willow Tohi
- New research suggests common dietary proteins like casein (from dairy) and wheat gluten can disarm cholera bacteria, reducing infection levels 100-fold in mice.
- The proteins work by jamming a syringe-like structure the bacteria uses to attack beneficial gut microbes.
- This food-based strategy offers a potential alternative to antibiotics, avoiding the risk of creating drug-resistant superbugs.
- Separately, the over-the-counter medication Pepto-Bismol (bismuth subsalicylate) is a proven, underutilized tool, reducing traveler’s diarrhea risk by 65%.
- Both findings highlight the growing importance of dietary and simple preventive strategies in combating infectious diseases.
In an era of antibiotic resistance and global disease spread, a powerful new line of defense against deadly infections may be found not in a high-tech lab, but in the kitchen pantry. Groundbreaking research from the University of California, Riverside, published in April 2026, reveals that ordinary dietary proteins can disarm cholera bacteria with startling effectiveness. This discovery, alongside the proven power of a simple, century-old stomach remedy, is reshaping the conversation on preventing infectious disease, emphasizing prevention through accessible, sustainable means.
The protein shield against an ancient scourge
Cholera, a waterborne bacterial disease that causes severe dehydration and can kill within hours, has plagued humanity for centuries. While modern sanitation and food safety measures have curbed its spread in developed nations, recent global surges have strained resources, highlighting the need for new strategies. The UC Riverside team set out to see if diet could be one such weapon. In a preclinical study using mice, they discovered that diets rich in specific proteins—casein from milk and cheese, and wheat gluten—reduced cholera colonization in the gut by up to 100-fold compared to other diets.
The mechanism is a molecular ambush. Cholera bacteria employ a microscopic, syringe-like structure to inject toxins into competing gut microbes. The researchers found that casein and gluten proteins effectively jam this syringe, disarming the pathogen. “We saw up to 100-fold differences in the amount of cholera colonization as a function of diet alone,” said senior author Ansel Hsiao. This suggests that, for vulnerable populations, dietary adjustments could serve as a crucial preventative buffer.
A safer path than pills
This research arrives at a critical juncture in public health. Overreliance on antibiotics has fueled the rise of drug-resistant superbugs. While cholera is still treatable with current medications, its adaptive nature poses a future threat. A dietary intervention sidesteps this risk entirely. “Dietary strategies won’t generate antibiotic resistance in the same way a drug might,” Hsiao noted. Using widely available, generally recognized-as-safe food proteins represents a potentially cheaper, more sustainable and scalable public health tool, especially in resource-limited settings where cholera often strikes hardest.
The study’s authors are clear that human trials are the essential next step to determine effective dosages and timing—whether the proteins work best as a daily preventative or as a treatment after exposure. Nevertheless, the principle it underscores is potent: the nutrients we consume can directly alter the battlefield within our guts, empowering our native defenses against invasion.
A pink bottle of prevention for the traveler
The concept of using simple, available substances for gastrointestinal protection is not entirely new. It finds a parallel in the robust evidence supporting bismuth subsalicylate, the active ingredient in Pepto-Bismol, for preventing traveler’s diarrhea. As highlighted in a March 2026 column by gastroenterologist Trisha Pasricha, this over-the-counter remedy can reduce the risk of acquiring this common vacation-ruiner by 65%. Despite its century-long history and strong clinical trial data, it remains an underutilized travel essential.
The protocol is specific: two tablets taken four times daily while awake, ensuring the protective compound is present in the gut when pathogens arrive. Unlike prophylactic antibiotics, it does not disrupt the gut microbiome or contribute to antibiotic resistance. Its side effects, like harmless blackening of the tongue or stool, are well-known. For travelers to high-risk regions, it represents a powerful, low-cost layer of defense that works in tandem with classic food and water precautions like avoiding buffets, unpeeled fruits and ice made from local tap water.
The historical shift from treatment to proactive defense
Historically, medicine has often focused on treating disease after it manifests. The growing understanding of the gut as a frontline immune organ, however, is driving a paradigm shift toward proactive, foundational support. The UC Riverside study on cholera and the well-documented efficacy of bismuth subsalicylate both exemplify this shift. They move beyond merely killing bad bacteria to instead neutralizing their weapons or creating an inhospitable environment for them. This approach aligns with a broader natural health principle: bolstering the body’s inherent resilience is often the most elegant and sustainable form of medicine.
A future fortified by food and simple remedies
While the cholera research requires further human validation, its implications are significant. It opens the door to exploring how other common dietary components might be harnessed to mitigate various infections. Combined with the forgotten efficacy of existing remedies like bismuth subsalicylate, it paints a picture of a more empowered public health future. In a world facing complex medical challenges, some of the most promising solutions may be found in re-examining the ordinary—the proteins on our plate and the pink liquid in our medicine cabinet. The path to preventing disease may increasingly be paved not just by advanced pharmaceuticals, but by the intelligent, strategic use of everyday resources.
Sources for this article include:
Submit a correction >>
Tagged Under:
cholera, cures, dairy, discovery, food cures, food is medicine, food science, grocery, gut health, healing, natural health, pantry staples, prevention, remedies, research, superbugs
This article may contain statements that reflect the opinion of the author
RECENT NEWS & ARTICLES
COPYRIGHT © 2017 REAL SCIENCE NEWS